7 mistakes we often make when talking about antibiotics
Misperceptions in the community about antibiotics are helping the actions that make the "nightmare" worse.
In these days, the global health crisis of antibiotic resistance has become the focus again. The genes for dangerous drug-resistant bacteria, even all the antibiotics we have, have been recorded in China, Europe, Canada and the United States.
Currently, there are up to 700,000 deaths globally globally caused by drug-resistant bacteria. Without action, the number will increase to more than 10 million by 2050.
The idea that this is a problem of the health system and the responsibility does not belong to each of us, however, the World Health Organization (WHO) survey shows that it is the misconceptions in the community about resistance Students are abetting the actions that make the "nightmare" worse. Here are 7 basic mistakes you can make when talking about antibiotics:
1. Antibiotic resistance will not happen if I choose the right medicine
False.
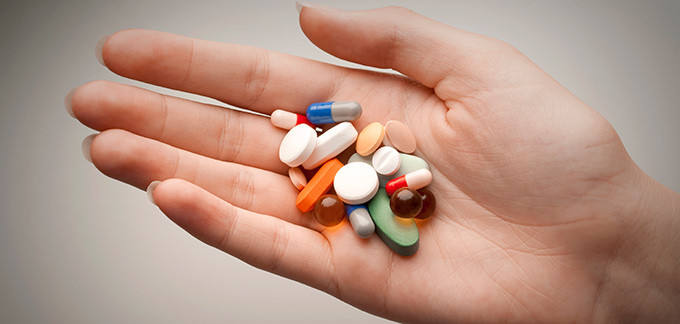
Antibiotic resistance has appeared before we invented antibiotics.
Antibiotic resistance occurs under the control of natural selection, as Darwin proposed in the theory of evolution. Bacteria, for thousands of years since birth, have to protect themselves from chemicals produced by other bacteria and fungi. In 1928, Alexander Fleming discovered this and us, simply calling those chemicals antibiotics.
Therefore, antibiotic resistance has appeared before we invented antibiotics. They must form resistance to survive and survive after an antibiotic attack, whether antibiotics come from mushrooms or from capsules that humans prepare.
Whenever we use an antibiotic, its resistance still occurs in bacteria. The fact that you choose a better drug, which doctors call "sensitive," only kills effectively the pathogenic bacteria that has not formed its resistance.
However, if there are unfortunately resistant bacteria, they will continue to survive and proliferate. The bacteria can exchange resistance to each other. This is one of the ways that resistant bacteria spread, especially in health facilities, when doctors do not comply well with hygiene regulations.
In short, even if you choose the right antibiotic, it is more "sensitive" but still capable of causing resistance.
2. My body is becoming resistant
Is not. The error is not yours, it's the bacteria.
Therefore, it cannot be conceived that changing something on the body will help us overcome resistance. The object you need to act on is bacteria.
3. Antibiotics will help you overcome colds and flu
False.

Antibiotics only work to fight bacteria.
Antibiotics only work to fight bacteria. Meanwhile, colds and flu are caused by viruses . Using antibiotics in this case is useless and counted as abuse. The more we abuse antibiotics, the more resistant bacteria are likely to be born and spread more.
Besides, using indiscriminate antibiotics also harms your body. The possible results if you use antibiotics to treat colds and flu are:
- Self-harming the body with antibiotic side effects
- Causing effects on spines and societies, when increasing the chances of resistance to bacteria
According to a WHO survey in 12 countries, up to 64% of respondents believe that influenza viruses can be treated with antibiotics. People with this point of view even force it on a doctor or nurse and ask them to prescribe antibiotics for themselves when they are sick.
Surveys also show that antibiotics are more abused in low-income countries. 42% of people in this area use antibiotics within 1 month before the survey. Meanwhile, only 29% in high-income countries.
4. During treatment, I can stop antibiotics on the last days
False.

Do not arbitrarily reduce the dose or stop using antibiotics without consulting your doctor.
Many people are suffering from this serious mistake, creating conditions for antibiotic resistant bacteria to develop. During treatment, they believe that they can reduce the dose or stop antibiotics once they feel better.
The truth is you are evaluating your condition according to your feelings. Symptoms are usually improved before a period of time, when the bacteria have been killed and processed by the body.
If you reduce the dose or stop using the antibiotic early, the amount of medication will not be enough to kill the remaining part of the bacteria. And no matter how much is left, they can still reproduce and reconstruct the population. As a result, the disease returned, while bacteria had more time to create resistance mechanisms.
So, the advice for you is to strictly follow your treatment regimen.Do not arbitrarily reduce the dose or stop using antibiotics without consulting your doctor.
5. I can use the other antibiotic of other people when not expired
False.

Never use excess pills.
Never use leftover pills in a family medicine cabinet, even if it comes from your own previous treatment.
There are two reasons for this:
- Antibiotics for others may not work for you, even if both are diagnosed the same.
- Antibiotics preserved over time may be reduced in activity and are more likely to cause resistance in bacteria.
6. Antibiotic resistance only occurs from the second course of treatment onwards
False.
As mentioned, antibiotic resistance can occur whenever you use antibiotics, even if it is the first time you treat this drug. Of course, there is a right logic here, the more times you repeat the treatment, the more likely the bacteria to be resistant to the drug.
7. Antibiotic resistance is the fault of the medical system
To be fair, antibiotic resistance occurs today, doctors and the health system have a great responsibility.
However, errors do not entirely belong to them. Ever since the first doses of penacillin were produced, Alexander Fleming warned of one day that the pills were no longer working.

We ourselves have to bear the rest of the responsibility for every abuse and consider antibiotics to be "miracles".
However, the failure to educate the community and raise our awareness of antibiotic use has made the situation worse than it is today. We ourselves have to bear the rest of the responsibility for every abuse and consider antibiotics to be "miracles". It is used indiscriminately for all diseases and even in livestock.
However, thinking now is no longer a time for us to blame each other. The key point now is that both the health system and the community must be responsible for the future of humanity. Antibiotics are a global benefit and it belongs to everyone, every generation.
What we do today is affecting the next generation. Therefore, this is a time when everyone needs to be aware of their antibiotic use, through proper awareness and action. Do not let mistakes on the hands of bacteria, making the "nightmare" worse.
- 5 common mistakes when using antibiotics
- Abuse antibiotics to make resistant bacteria
- Why do we repeat mistakes?
- What are antibiotics and classify antibiotics
- 'Heavenly' facts about antibiotics
- Find new antibiotics under the ocean
- The most frightening mistakes of humans
- Abuse of antibiotics will make children more susceptible to illness
- Harm when doing many things at the same time
- Why do you know that antibiotics do not treat flu, many people continue to abuse?
- Na main case, how much appetite should avoid these mistakes when eating
- Antibiotics from dirt
 The United Nations' all-human warning: All antibiotics are becoming useless
The United Nations' all-human warning: All antibiotics are becoming useless How did bacteria learn to fight antibiotics?
How did bacteria learn to fight antibiotics? 10 million deaths are one of the startling numbers about 'Antibiotic resistance'.
10 million deaths are one of the startling numbers about 'Antibiotic resistance'. Learn about the phenomenon of antibiotic resistance
Learn about the phenomenon of antibiotic resistance