The abnormality of cancer: When the lungs turn into stomach and intestines
We know cancer is a defect in the body's genetic system. Therefore, it is not surprising that the environment inside the tumor becomes a place for extremely unusual things to happen.
One of the super phenomena of cancer was discovered in 2018, when scientists observed the stomach, duodenal and small intestine cells inside the lung tumor.
What happen? Did these cells run from one part of the body to another and reside in cancer tumors?
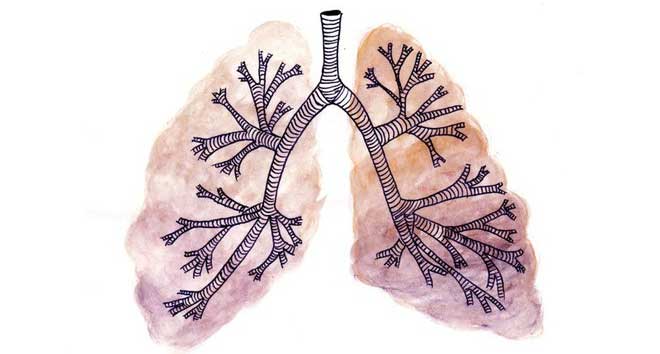
When lung cells have cancer, they turn into stomach cells
The answer is: No! Lung cancer cells have turned into cells of the organ next to them. This happens because cancer has turned off a gene labeled NKX2-1 that controls the development of lung cells.
Without this gene, the stem cells in the lungs will not develop to become lung cells themselves, but will be abandoned and " lost " in the pathways of the cells of nearby organs. They have turned into stomach cells, small intestine and duodenum.
The findings, published in the journal Developmental Cell, emphasize the flexibility of cancer cells. Attack on NKX2-1 gene allows lung cells to transform , which is resistant to drugs that treat lung cancer.
" Cancer cells will do anything to survive ," said Purushothama Rao Tata, a research author at Duke Medical University. "In the face of chemotherapy drugs, lung cells turn off its important properties and load on the properties of other cell types to resist resistance to drugs."
Spending most of his career researching lung cells, Professor Tata found that these cells often possess highly flexible metamorphic mechanisms after injury.
He began to wonder: Are these mechanisms also causing chaos in lung cancer tumors? Professor Tata decided to focus on understanding this in non-small cell lung cancer tumors, accounting for 80-85% of all cases of lung cancer.
In fact, lung cancer is the leading killer in the world. Lung cancer patients have the lowest survival rate of all types of cancer.

Lung cancer is a mess of different types of cells belonging to many different organs.
Professor Tata analyzed data from the Atlas Cancer Genome Research Network, a large group that is storing the genome of thousands of cancer samples from 33 different types. He found a large proportion of non-small cell lung cancer tumors do not have NKX2-1, a specific gene used to identify lung cells.
Instead, many tumors express some genes of esophageal cells and other parts of the gastrointestinal tract. One hypothesis is set out to explain, when lung cancer cells lose the NKX2-1 gene, it will be able to transform to take on the characteristics of other organ cells.
In fact, lung cells and intestinal cells grow together from a parent cell, its precursor cells. Therefore, when genes are lost, lung cells are more likely to develop along their sibling's path, turning into cells of other organs.
To test whether this is true, Professor Tata and colleagues removed the NKX2-1 gene from lung cancer tumor tissue of experimental mice. They then monitored the development of these tissues under a microscope.
As expected, tumor cells exhibit some common characteristics only in intestinal cells, such as cavity structure and stomach tissue. More surprisingly, these structures also produce digestive enzymes, as if they were in the stomach and not the lungs.
After pointing out a simple genetic change that could motivate lung cells to change their path of development, Professor Tata wondered if another tweak could make them cancer. This time, in addition to removing NKX2-1 gene, the team activated two oncogene genes SOX2 and KRAS.
As a result, mice with SOX2 mutations developed tumors as if they were in the head of the gastrointestinal tract, from the mouth to the duodenum. Mice with KRAS mutations developed tumors similar to tumors in the middle of the gastrointestinal tract to the anus.

Lung cancer cells can turn into other organ cells, to resist specific drugs for lung cancer.
" Cancer biologists have long suspected that cancer cells can mutate to resist chemotherapy, but they don't know the mechanism behind that flexibility ," said Professor Tata. .
" Now we know we are dealing with these tumors [lung tumors are capable of transforming into other forms] - we can think of the paths that these cells can convert and design therapies to stop them " .
In the future, Professor Tata plans to use his lung tumor model to discover more mechanisms of resistance to this dangerous cancer.
Once the therapies are successfully developed, we can reduce the rate of chemotherapy resistance of lung cancer tumors, thereby improving the prognosis and survival ability of patients.
- Stomach cancer is detected through breathing
- Create the stomach in the world's first laboratory
- Want to avoid the second most dangerous cancer in Vietnam, remember this eating habit
- Detection of the gene causes breast cancer to spread to the lungs
- New evidence of the benefits of breast milk
- Nano-electronics can detect the risk of stomach cancer
- Preventing stomach cancer from coffee
- Add a simple measure to prevent stomach cancer
- Create artificial lungs to test the treatment of lung cancer
- Protein discovered to prevent stomach cancer from spreading
- Can detect 5 types of cancer at the same time with just one drop of blood
- Vietnamese people eat and drink together and are susceptible to infection causing stomach cancer
 New drug causes cancer to 'starve'
New drug causes cancer to 'starve' Why is Australia the country with the highest cancer rate in the world while Vietnam ranks 100th?
Why is Australia the country with the highest cancer rate in the world while Vietnam ranks 100th? Common cancers in men
Common cancers in men America's incredible discovery: The most feared cancer cell is love
America's incredible discovery: The most feared cancer cell is love