Strains of flesh-eating bacteria combine to cause a deadly infection
According to a study published in the Proceedings of the US National Academy of Sciences (PNAS), two strains of predatory bacteria can work together to cause maximum damage to the human body.
This process is discovered after an infected patient who has had to undergo a four-part resection during treatment after the disease becomes dangerous.
"Now we have the ability to identify strains of a bacterial species, and it is very likely that we will find that multicellular infections are very common," co-author Rita Colwell, University Professor at University learn Maryland speak.
The patient described in the article was diagnosed with necrotizing fasciitis, a rare but potentially fatal infection requiring treatment and surgery, using rapid antibiotics. According to the Centers for Disease Control and Prevention (CDC), one in three people treated for the disease will die. Others may have lifelong disabilities.
In this case, doctors used traditional diagnostic methods to identify the bacteria that caused the Aeromonas hydrophila infection, and were surprised when the patient's condition had to be amputated. save.
Only when the authors of the study completed the genetic analysis of the patient's bacterial culture did they identify different strains in the culture medium.
"This study provides clear evidence that a very serious infection considered to be due to a species of natural bacterium actually has two strains," Colwell said in a statement.
"One of them produces a toxin that breaks down muscle tissue and allows another strain to move into the blood system and infect organs."
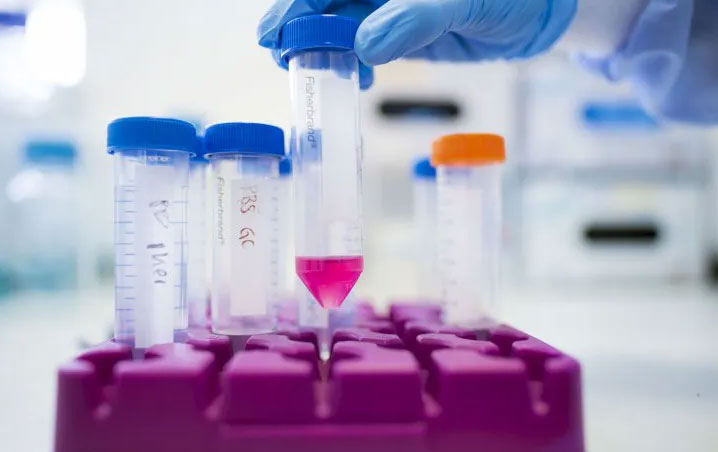
The study describes how two strains of predatory bacteria work together to cause maximum damage.
Previous studies have shown that not one but two strains of Aeromonas hydrophila can cause skin necrosis - muscle 1 (NF1) infection and necrotizing fasciitis 2 (NF2). When either strain interacts with the human body in different ways, they do not seem to cause a deadly infection. Only when both strains are present and cooperate will the most dangerous infection occur.
Colwell and colleagues used a mouse model to determine how gene regulation for NF1 and NF2 could affect the ability to infect and interact with each opposing strain.
The results showed that NF1 itself would be in a position until processed by the body's immune system. When NF2 releases toxins that weaken muscle tissue itself, it can spread to other parts of the body. But when both are combined, NF2 will break down muscle tissue and NF1 will spread. NF1 kills NF2 so the strain is then confined to one place. In contrast, NF1 becomes more dangerous and can be life-threatening in human hosts.
This may explain why antibiotics in these cases will not be effective."When we treat with a certain antibiotic, we remove a strain of bacteria from the body," Colwell said. "But if another organism were involved in the infection and caused the disease, any non-targeted antibiotic treatment would probably cause it to grow that way . " Instead, Colwell said that a combination of antibiotics and other drugs would work.
The results of the study reject the traditional assumption that infections are caused by a single cell caused by a single strain of bacteria. Studies show that infections that are difficult to treat and progress quickly are caused by strains of bacteria interacting with each other instead of a single strain.
Another example is reported: Campylobacter jejuni - a bacterium that can cause food poisoning, and Pseudomonas putida - a bacterium that manages oxygen levels together to cause an uncomfortable stomach disease. .
- American doctors are concerned about a new deadly fungal infection strain
- Alarm on E.coli strain ST131
- Close up of beautiful deadly bacteria surprised
- Deadly bacteria attack Europe again?
- Improper washing of chicken can spread deadly bacteria
- The deadly bacteria in this day can explode when antibiotic resistance comes
- What kind of bacteria can kill hundreds of millions of people coming out from the North Pole?
- There is an uncontrollable spread of bacteria
- The mystery of alien strains is already on Earth
- Treatment of polluted water with microorganisms
- Warn predatory bacteria to attack during the rainy season
- Artificial nose helps to find blood infection bacteria
 Why do potatoes have eyes?
Why do potatoes have eyes? 'Tragedy' the world's largest carnivorous life: Death becomes ... public toilet
'Tragedy' the world's largest carnivorous life: Death becomes ... public toilet Tomatoes were once considered 'poisonous' for 200 years
Tomatoes were once considered 'poisonous' for 200 years Detecting microscopic parasites on human face
Detecting microscopic parasites on human face